Hypoxic-ischemic encephalopathy, a form of brain damage, is often caused by unnecessary delivery trauma. When obstetricians fail to uphold their duties, our attorneys step in to pursue justice.
- Decades of trusted trial experience protecting children.
- Our attorneys have secured millions for families.
- Call our lawyers today to receive a free consultation.
Our experienced birth trauma lawyers help families pursue justice – and compensation – every day. Protecting your child’s rights is our only goal.
Doctors must do everything in their power to prevent unnecessary harm. That legal duty is no more important than when a child’s life and well-being are on the line.
"Intelligent" He's a skillful negotiator, who instinctively reads a situation correctly, truly a great guy.
Birth asphyxia puts nearly every one of an infant’s organs at risk, but brain damage is almost certainly the most serious consequence. When infants are deprived of oxygen shortly before or during delivery, the result is often a brain injury known as hypoxic-ischemic encephalopathy, or HIE. Children who have sustained brain damage during labor or delivery can develop severe, and lifelong, disabilities, including developmental impairments and the neurological disorder cerebral palsy.
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
To understand this little-known, but often devastating, form of birth injury, let’s look at what hypoxic-ischemic encephalopathy actually means:
- Hypoxia – a drop in the amount of oxygen reaching body tissues
- Ischemia – a decrease in blood flow to the organs
- Encephalopathy – disorder or disease of the brain
As we can see, HIE is a type of brain damage caused by oxygen deprivation, compounded by a severe decrease in blood circulation.
How Hypoxic-Ischemic Encephalopathy Works
When a child is cut off from oxygen, even momentarily, the infant’s body goes into overdrive, attempting to stave off damage to organs and tissues for as long as possible. Redirecting blood flow is of primary importance. Under normal circumstances, the child’s body will quickly reroute its blood supply to nourish the most crucial organs first. Along with the adrenal glands and heart, the brain receives a significant increase in blood supply, according to the University of Chicago. This allows brain cells to survive for a time.
When a newborn suffers hypoxic-ischemic encephalopathy, however, this fall-back strategy isn’t always possible. With blood flow decreased for some reason, the cells that make up the brain can’t be nourished by an adequate supply of oxygen and soon die. This cellular die-off is the first and most extensive cause of brain damage during a hypoxic event, but researchers actually define a second stage of HIE, which can continue to cause further brain damage long after an infant’s delivery.

Without adequate oxygen, brain cells aren’t able to dispose of their waste products appropriately. These toxins build up, and can lead to cellular damage. Even when the cells survive, restoring proper blood flow to the brain isn’t a simple solution. An influx of blood forces these damaged cells to release their toxins, leading to a “reperfusion injury” which can last for days, or even weeks, after delivery.
Neonatal Brain Injuries: Early Warning Signs
Hypoxic-ischemic encephalopathy is a specific clinical syndrome, one that obstetricians may be able to diagnose soon after birth by observing the following symptoms:
- Depressed consciousness (lasting from one to two weeks)
- Hypotonia, or low muscle tone
- Inability to feed
- Seizures and epileptic brain activity
Despite these general diagnostic criteria, it’s important to note that the signs of infant brain damage can vary widely, depending on which portions of the brain have been injured and how long the organ was deprived of oxygen. Some children will fit the classical description of HIE, but others won’t.
Additional symptoms of hypoxic-ischemic encephalopathy can include:
- Low breathing rate
- Impaired reflexes
- Cyanosis – a bluish tinge to the skin caused by lack of oxygen in body tissues
- Acidosis – an increase of acids, either in the blood, body tissues or both
- Low Apgar scores
The vast majority of physicians, however, don’t rely on physical signs to diagnose a case of hypoxic-ischemic encephalopathy. Instead, doctors generally turn to a battery of diagnostic tests, like MRI and ultrasound, to monitor an infant’s brain activity and functioning.
Can We Treat Hypoxic-Ischemic Encephalopathy?
After being delivered, many infants who have suffered brain damage will need to be resuscitated, especially newborns who have been deprived of oxygen.
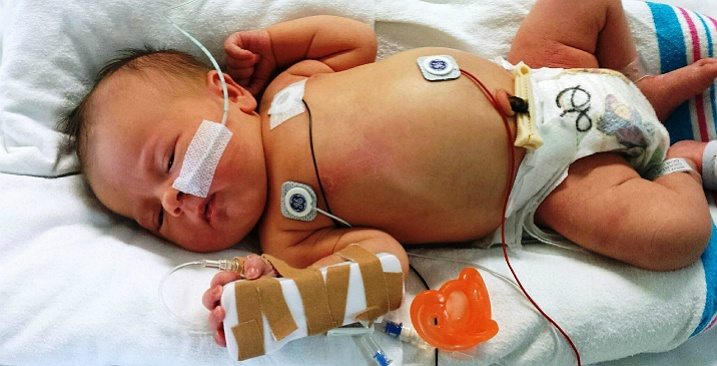
Once the child has been stabilized, doctors will attempt to prevent continued brain damage, while providing support to the infant’s organs. In many cases, a mechanical ventilator will be employed to breath for the child, and some newborns will need to be placed on mechanical ventilation for days. Meanwhile, doctors will closely monitor the infant’s cardiovascular functioning for signs of abnormal blood glucose levels.
Many children with HIE will experience seizures, and managing these episodes of abnormal brain activity is crucial. Seizures can lead to further brain damage and also threaten the lungs and heart. Anticonvulsant pharmaceutical drugs are usually prescribed at this time.
Hypothermic Treatment
Hypothermia therapy is a recently developed, but increasingly common, treatment for children who have sustained hypoxic-ischemic encephalopathy. Doctors lower the infant’s body temperature under controlled conditions to slow down cellular activity. This allows brain cells more time to recover from their injury.
According to researchers at Medscape, a wealth of experimental research shows that mild hypothermia – lowering a baby’s temperature by around 3 to 4 degrees Celcius – can significantly improve outcomes. But there’s only a short window to implement the treatment, which works best within the first six hours after a child’s delivery.
Many researchers say that hypothermia is the only effective treatment for infants with HIE. In fact, failing to appropriately administer hypothermia therapy after an infant has been diagnosed with hypoxic-type brain injuries may itself constitute medical negligence.
Effects Of Hypoxic-Ischemic Encephalopathy
While some brain injuries caused by birth asphyxia will lead to only minor impairments, hypoxic-ischemic encephalopathy can be fatal, usually due to massive organ failure. Medscape reports that broad estimates in the medical literature place the fatality rate for children who have suffered severe HIE between 25% and 50%. Every year, hypoxic-ischemic encephalopathy brain injuries contribute to more than 800,000 infant deaths. Those children that survive can develop a range of neurological disorders, from cerebral palsy to epilepsy. Only around 10% of infants who experience severe HIE will not develop some form of complication. As you would expect, the prognosis for mild cases of hypoxic-ischemic encephalopathy is much better. Children who develop only minor brain injuries usually aren’t affected by long-term central nervous system disorders.
What Causes Infant Brain Damage?
Hypoxic-ischemic encephalopathy is a leading cause of brain disorders among infants. Some estimates attribute up to 75% of all neurological impairments in newborns to hypoxic-type brain injuries, in which a newborn’s vulnerable brain is starved of oxygen. But what causes HIE in the first place?
Most cases of hypoxic-ischemic encephalopathy develop during or just before an infant’s delivery, and a host of different factors can be at play:
- Physical trauma inflicted during delivery
- Excessive oxytocin, a hormone used to stimulate contractions
- Umbilical cord problems, including knots and prolapse
- Long, protracted deliveries
- Placental abruption – when the placenta peels away from the uterine wall prematurely, cutting off a fetus’ blood and oxygen supply
- Shoulder dystocia – a complication of delivery in which a child’s head emerges from the birth canal, but his or her shoulders remain stuck behind the mother’s pelvis
- Placental blood clots
- Maternal infections
- Blockage of infant’s airways
- Infant anemia
Some cases of HIE are likely due to preexisting maternal health conditions, like low blood pressure, which can reduce the amount of oxygen delivered to a growing fetus. Doctors, of course, have a duty to diagnose and appropriately treat these medical conditions in a timely fashion, so as to avoid harm to both child and mother.
Even so, many cases of birth asphyxia are truly unavoidable, leaving few options for even the most skilled healthcare professionals. Some infants are born with serious lung disorders, conditions that developed during their time in the womb. There may be no way for doctors to treat these congenital disorders until after a child has been born.
When Medical Negligence Causes Brain Injuries At Birth
But many of the situations we’ve covered are true emergencies, and physicians, midwives and nurses must act swiftly to prevent severe harm befalling an infant. For some families, these essential medical interventions never come, despite all signs pointing to their absolute necessity.
Other causes are clearly negligent. Doctors make mistakes. We all know that. But when negligent medical decisions lead to neonatal brain damage, acknowledging a mistake isn’t enough. Families deserve support, especially families raising children who sustained birth injuries. Legal action is one possibility, and if a child’s condition was caused by medical malpractice, families may be entitled to significant financial compensation.



