A new study has found further evidence to support the current clinical guidelines for the use of hypothermia therapy in newborn babies who have endured hypoxic-ischemic encephalopathy, a form of brain damage caused by oxygen deprivation.
Testing The Limits Of Hypothermia Therapy
Newborns who develop hypoxic-ischemic encephalopathy, a form of brain damage linked to oxygen deprivation, often go on to develop serious neurological disorders, including cerebral palsy and seizure disorders. Severe cases of brain damage can be fatal; between 15% and 25% of children with hypoxic-ischemic encephalopathy, or HIE, will die before reaching the age of four weeks. Worldwide, nearly 1 in 4 of the 4 million neonatal deaths every year are linked to the signs of birth asphyxia, according to expert authors writing in the Nelson Textbook of Pediatrics.
How Therapeutic Cooling Works
Hypoxic-ischemic encephalopathy is a major problem. That’s why the medical community met hypothermia therapy (or “targeted temperature management”) with such excitement.
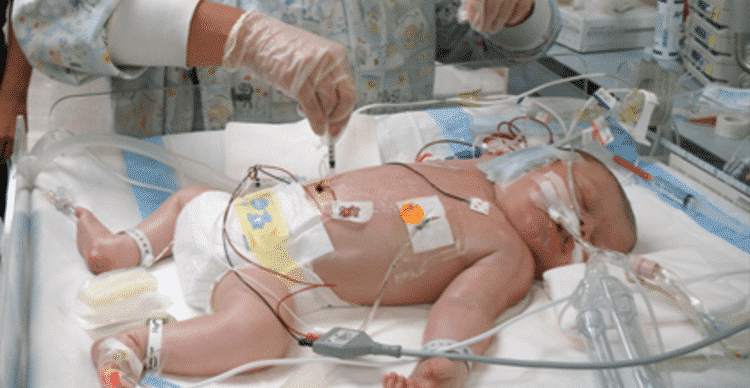
The treatment is, in theory, extremely simple, although researchers only began studying its effect on infant brain damage in earnest during the 1950s. Artificially cool an infant’s body temperature directly after birth and the physical processes leading to brain cell death slow down.
The result? Deaths drop dramatically; thousands of children are saved. Permanent brain damage and long-term disability can, in many cases, be avoided.
Current Clinical Guidelines
Hypothermia therapy is a revolutionary new treatment. Doctors are still trying to find out exactly how it works. The most-comprehensive study on the therapy’s benefits included only 208 children and was published just five years ago. However new the science, obstetricians around the world have already latched onto hypothermia therapy as a critical treatment method, even developing standardized guidelines to help physicians in the clinical setting.
As Neurology Advisor notes, the standard of care for administering hypothermia instructs physicians and nurses (usually working in a neonatal intensive care unit) to cool an infant’s core temperature to a target of 33.5°C (92.3°F) for a total of 72 hours. Doctors generally agree that hypothermia treatment is most effective when initiated within six hours of a child’s birth.
These guidelines have certainly saved numerous children, but doctors have long been interested in what seems an intuitive hypothesis. Could longer periods of cooling, or lower temperatures, reduce the risk of long-term brain damage even more?
Study Team Tries Lower Temperatures, Longer Times
To find an answer, a large team of researchers from 24 different research institutions (both academic and governmental) set up a randomized clinical trial, in which babies who had suffered hypoxic-ischemic encephalopathy would receive hypothermia treatments at lower temperatures, and for longer periods of time, than the currently-accepted clinical standard.
Study Design
364 newborns were eventually enrolled in the study. Each baby was assigned to one of four possible treatment regimens:
- 33.5°C for 72 hours (current clinical guidelines)
- 32.0°C for 72 hours
- 33.5°C for 120 hours
- 32.0°C for 120 hours
After treatment had been administered, the researchers followed those infants who survived their condition for an average of 20.7 months. The question, of course, was whether or not moderate or severe disabilities would be less common among babies who received hypothermia therapy outside the clinical standard, for longer time periods, at lower temperatures or both.
They weren’t.
Deviations From Clinical Standard Don’t Provide Greater Benefits
After adjusting the results to account for variations in brain damage, the researchers found that lower temperatures and longer periods of cooling appeared to have no beneficial effect.
Children cooled at 32.0°C, 1.5° lower than the clinical guideline, died or developed disabilities at the same rates as children who received the standard treatment. The same was true for babies who were cooled for 120 hours. Infants exposed to both lower temperatures and longer times developed fewer disabilities, but died at higher rates than their peers.
On balance, the researchers concluded that “the current regimen of cooling for 72 hours at 33.5°C” was still the best choice for children.
No Impact On Long-Term Outcomes
Changes in temperature and time period had almost no effect on any of the study’s secondary outcome measures, either:
- death after being discharged from the NICU
- rehospitalization
- disability level
- visual, auditory and multiple disabilities
- cognitive and motor function test results
- cerebral palsy rates
- abnormal growth rates
At least for now, the clinical guidelines for hypothermia therapy have survived critical scrutiny. Now because this study is small, only 364 babies, its results shouldn’t be taken as conclusive.
Larger patient groups may be able to find evidence of more-nuanced changes in the rates of death and severe neurological impairment. Despite this qualification, the results are largely consistent with previous findings, along with the current clinical guidelines that have emerged from the medical community. The results were published in the Journal of the American Medical Association on July 4, 2017.


